Medtronic Global Lung Health Summit Inspires Bold New Plan For Treatment of Lung Cancer
Kootenai Health’s continuum of care approach is making a difference for patients in northern Idaho.
“I can do more for these patients,” thought Dr. Todd Hoopman, medical director for the lung nodule program at Kootenai Health in northern Idaho.
Inspired by what he had just seen and heard at the 2016 Medtronic Global Lung Health Summit, Dr. Hoopman spent his entire flight home writing. First, he spent two hours “feverishly” drafting a new plan for 2018 and beyond.
Then, Dr. Hoopman fired off an email to the Medtronic Lung Health team. In it, he vowed to “do more” and described his new vision: “It is bold. It is different than anything else currently occurring at Kootenai Health. It is going to be a difficult sell to all the involved parties. But ‘it’ is going to make a difference.”
Combatting Lung Cancer, Together
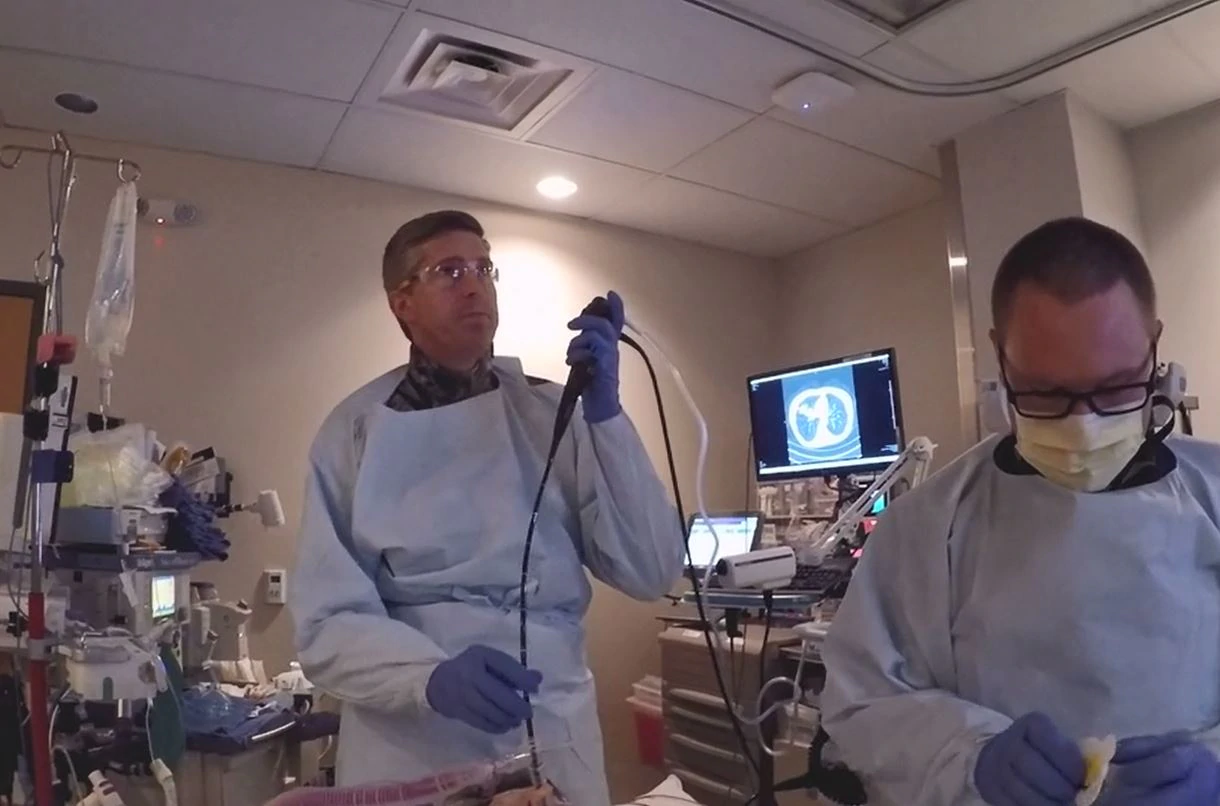
As a first step, Dr. Hoopman assembled a team of nurses, surgeons, and hospital administrators focused on a singular goal: to catch lung cancer earlier. Offering navigational technology* to aid physicians in the visualization of the lung — and by providing lung health expertise through its Impact Program — Medtronic then helped the team identify ways to improve the entire continuum of care — from detection to treatment. The Impact Program is intended to foster collaboration across specialties, help create processes, and help identify key metrics as a hospital staff builds out its lung health program.
The Kootenai team’s goal was to create a better way to screen, track, and treat more lung cancer patients — earlier.
Especially those with an incidental diagnosis.
An incidental diagnosis occurs when a lung nodule is identified during treatment for a different illness or injury. Patient Carl Blish, for example, saw his doctor following a slip on the ice. The CT scan to look for broken ribs revealed something else entirely: a spot on his lungs.
“I was shocked,” Carl recalls. “Physically, I hadn’t felt anything at all.”
“Patients often come to our attention through the discovery of incidental nodules,” says Dr. Hoopman. But, he says, those patients can easily fall through the cracks. “They typically aren’t tracked well and sometimes don’t even know they need treatment. Now, we have a way to track — and effectively treat — these patients.”
Meeting a need
Too often, lung cancer is caught in stages three and four when treatment options are limited.1 What’s more, treatment of late-stage nodules is 300 percent costlier than it is for cancers caught at an earlier stage.2 But early detection, diagnosis and treatment of lung cancer can improve outcomes and lessen the disease’s economic burden.
Plus, patients want a more streamlined process. A recent study, which surveyed hundreds of cancer patients, found that services related to convenience and coordination ranked as their highest needs.3
The team at Kootenai Health improved communication between pathologists, pulmonologists, interventional radiologists, oncologists, and cardiothoracic surgeons. And each patient gets a “nurse navigator” to guide them along the often-complex treatment journey. “Medtronic hasn’t been about equipment only,” says Cori Sowa, the team’s thoracic nurse navigator. “Their goal is to help us expand this program and help patients along the entire continuum of care.”
Today at Kootenai Health, patients are tracked, diagnosis happens quickly, surgery is scheduled, and the patient is supported along the way.4 Since this enhanced lung health program was launched, the team has seen a yearly increase in the number of incidental cases identified and tracked, and has shortened the diagnosis-to-treatment timeline significantly.
“We couldn’t do this alone,” says Dr. Hoopman. “The level of support I’ve gotten from Medtronic has been unparalleled.”
Today, Carl’s lung cancer is gone. And stories like his are the reason the Kootenai Health team isn’t slowing down anytime soon.
“This is what we’re meant to do on this team,” says Dr. Hoopman. “We’re excited about the future.”
And Dr. Hoopman was right: his bold plan is making a difference.
*Important Safety Information
Indications for use are:
superDimension™ navigation system
Indications for Use
Indicated for displaying images of the tracheobronchial tree to aid the physician in guiding endoscopic tools or catheters in the pulmonary tract and to enable marker placement within soft lung tissue. It does not make a diagnosis and is not an endoscopic tool. Not for pediatric use.
See product labeling for relevant contraindications, warnings and precautions.
Federal law (USA) restricts this device to sale by or on the order of a physician.
Contraindications
Flexible bronchoscopy should be performed only when the relative benefits outweigh the risks.
Absolute contraindications include, but are not limited to:
- Absence of consent from the patient or his/her representative, unless a medical emergency exists and the patient is not competent to give consent.
- Absence of an experienced bronchoscopist to perform or closely and directly supervise the procedure.
- Lack of adequate facilities and personnel to care for emergencies such as cardiopulmonary arrest, pneumothorax, or bleeding.
- Inability to adequately oxygenate the patient during the procedure.
- Pediatric patients.
- The safety of use of the superDimension navigation system in patients with electrically or magnetically activated implanted medical devices has not been evaluated.
The danger of a serious complication from bronchoscopy is especially high in patients with the disorders listed below. These conditions are usually considered absolute contraindications, unless risk-benefit assessment warrants the procedure:
- Coagulopathy or bleeding diathesis that cannot be corrected.
- Severe obstructive airways disease.
- Severe refractory hypoxemia.
- Unstable hemodynamic status including dysrhythmias.
Relative contraindications or conditions involving increased risk, according to the American Association for Respiratory Care (AARC) (Respir Care. 2007 Jan;52(1): 74-80) for Fiber-optic Bronchoscopy in adults, include:
- Lack of patient cooperation.
- Recent myocardial infarction or unstable angina.
- Partial tracheal obstruction.
- Moderate-to-severe hypoxemia or any degree of hypercarbia.
- Uremia and pulmonary hypertension (possibility of serious hemorrhage after biopsy).
- Lung abscess (danger of flooding the airway with purulent material).
- Obstruction of the superior vena cava (possibility of bleeding and laryngeal edema).
- Debility, advanced age, and malnutrition.
- Respiratory failure requiring mechanical ventilation.
- Disorders requiring laser therapy, biopsy of lesions obstructing large airways, or multiple transbronchial lung biopsies.
- Known or suspected pregnancy (because of radiation exposure).
The safety of bronchoscopic procedures in asthmatic patients is a concern, but the presence of asthma in most cases does not preclude the use of these procedures.
1Morgensztern et al. J Thoracic Oncology. 2010;5:30.
2Gildea et al. (2017). ClinicoEconomics and Outcomes Research. 9: 261:269.
3“What do Cancer Patients Care About Most?” The Advisory Board Company: Oncology Roundtable.
4Based on Kootenai Health data. Data on file.